I spent three hours yesterday attending a meeting of PAR Ohio, learning about the brokenness of systems meant to respond to heroin. The best I can say is that things here are at the starting point.
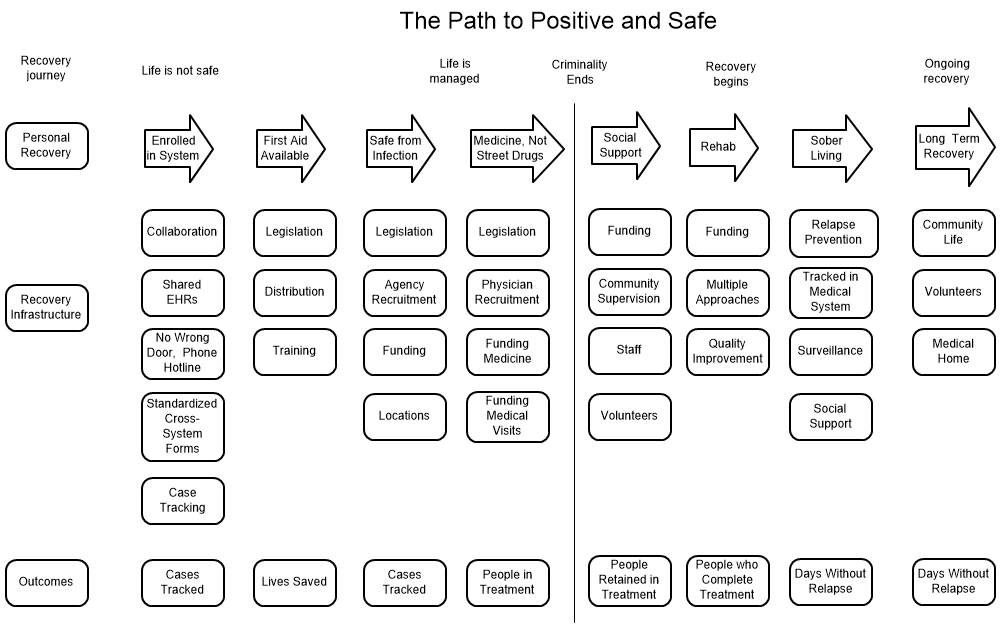
Here's the lowdown, in snapshot format, following the milestone and infrastructure model in my book Sharp Stop Heroin and Rescue People.
Date: December 19, 2014
Community: Southwestern Ohio
Author: Paul Komarek
Extent of problem
Severe.
Enrolled in System
The “system” in place is largely irrelevant to public service needs. The public’s experience is chaotic and disorganized. Very few people know how to access basic system resources.
Hamilton County has a designated “front door” for recovery services, but no one mentioned it in the course of a three hour public meeting.
There was some knowledge of Medicaid, but no generally known single point of contact for enrollment, and no readily available resource. Ohio’s Medicaid system is in peril, in any event.
Emergency treatment systems are poorly understood. Ohio has multiple overlapping mandatory treatment statutes, and each county has a different process. Some courts have forms, others don’t. None of them are organized in such a way as to solve the entire problem of someone who needs immediate care because they pose a danger to self or others.
Criminal justice service systems are not connecting with treatment resources. Jails are the de facto detox resource for the community, but the largest jail provides no detox medication support.
Primary care systems are not connecting with treatment systems.
The treatment landscape is entirely different in each of four SW Ohio counties. Each county has opiate task forces working on local approaches to problems, but they are lunging after one solution or another, not working regionally, and doing whatever they prefer. They actually compete against each other for scarce grant funding resources. Ohio’s Medicaid behavioral health carveout makes this worse, and slows the development of effective regional systems and access to new resources.
Ohio’s Medicaid plan needs updating, and will not be effective until it accommodates all levels of care.
Apart from the VA, Ohio treatment organizations are not systematically integrating behavioral health electronic health records with commercial systems.
First Aid Available
Naloxone prescriptions are available, but there is uncertainty around obtaining the actual kits. Opiate prescribers are not routinely prescribing Naloxone. The proper legislation is in place.
Safe from Infection
Syringe exchange is available during restricted hours in two Cincinnati neighborhoods. It is not available in the suburbs.
Medicine, Not Street Drugs
Methadone is available, but the general public objects to it. Some dispensaries are reportedly not moving people towards dose reduction. Suboxone is available, but Ohio Suboxone prescribers are requiring Medicaid patients to pay hefty fees for clinical services. Vivitrol is available, but mostly at the jail door, dispensed to released prisoners, and paid for by grant funding. There is poor public understanding of the role of medication in opiate treatment, especially around the notion of appropriate medication use for years or even for a life time. Local jails do not support medication assisted treatment.
Social Support
Cincinnati has an active AA/NA community, with several hundred meetings each week. There is very limited access to secular support (Women for Sobriety, SMART, LifeRing). The AA/NA community is positioned as anti-medication, especially methadone. The public is advocating for detox, not medication assisted treatment, despite the research on effectiveness of MAT. People who use MAT are shamed in AA/NA groups. Local faith-based groups are not stepping forward to support people in recovery.
Rehab
Rehab resources exist, but are not accessible without sponsorship or substantial external funding. Ohio Medicaid does not pay for inpatient rehab. There is insufficient variety and personalization with respect to treatment approach. No one is managing or balancing available system resources. There may nominally be “plans” but they are not focused on what it takes to actually solve the problems.
Sober Living
There is a severe shortage of recovery housing. What exists is explicitly 12-step based, which presents difficulties for people who use medication assisted treatment.
Long-Term Recovery
Relatively few people experience true recovery under the existing Ohio “system.” Evidence-based resources for people with complicated sets of problems are essentially nonexistent. The mental health system is overtly oriented towards managing the lives of dependent, non-addicted populations with high levels of disability burden, not those dying in high numbers today.
Ordinary people help each other cope with tough issues like depression, addiction, trauma, anxiety disorder, PTSD, and schizophrenia every single day in every culture on earth.
Dec 19, 2014
Dec 7, 2014
Heroin W.M.D.
 Heroin is not that complicated. It’s a weapon of war, part of an invasion that delivers a plague.
Heroin is not that complicated. It’s a weapon of war, part of an invasion that delivers a plague.Our mission is relatively simple: Repel the invader. Save the people.
Anything else plays into the enemy’s hands.
The drug cartels are clever and heartless. They exploit our vulnerabilities, and make us complicit in our own destruction. They use people with economic vulnerabilities to sell drugs to people with health vulnerabilities. When we jail our own children, it produces more business for our enemies.
“Friend or foe?” and “What can I do to help you?” are key questions. They help us stop the damage.
The neighbor kid with the needle in his arm passed out on the floor is not the enemy. The kid on the street corner with packets of drugs in his pocket is not the enemy. Both are pawns, people who've been hijacked by the invader. It's better to protect them. They both need a path from drugs, a way to return to us. One needs treatment The other needs a real job.
Sure, both are technically criminals. Big deal. People can change under the right conditions. We know how to help, and we know prisons and jails waste people. With heroin, we are facing an invasion. The larger goal is more important. We can’t afford to overlook opportunities to save vulnerable people.
Smart legislation, smart court rules, smart diversion programming, smart discretion at time of arrest, smart bail policies, smart probation services all save people. They are investments that lower the body count. And they limit collateral damage -- the families and communities who suffer too. Besides, people who overcome challenges become more resilient. When people reach their ultimate potential, our society wins.
If we become become smart about criminal justice, recovery becomes our counterattack. Given what we are facing, smart justice may well be the key to victory.
---
Join me 9 am - noon on Saturday December 13 at the PIER in Newport KY for "A Course About Solutions." It's a 3-hour class about heroin and public policy.
Learn more at http://www.SharpStopHeroin.com
or RSVP at http://www.meetup.com/SHARP-Stop-Heroin-Study-Group/events/218807100/
Oct 25, 2014
Separated Orphan Twins
In 2014 my work focused on addiction, specifically on the heroin epidemic claiming so many lives across the U.S. My new book SHARP Stop Heroin and Rescue People reflects that work.
That work helped me to focus more on the question of integrated care. Poor social choices and bad public policy have caused mental health and addiction care to develop like separated orphan twins.
Mental health and addiction are both biopsychosocial, with biological, psychological, and social aspects that continuously reinforce each other and cannot be easily separated, but the treatment systems are separated. Over the course of decades, each system figured out how to emphasize and advocate for its particular service delivery style, treatment philosophy, and culture of care.
This has caused clinicians to develop blind spots. People come away with a different diagnosis and different treatment depending on the system they walk into.
The separation has affected the overall health of the population using mental health and addiction services. We see this in the resistance of addiction treatment systems to medicine-assisted addiction treatment. We also see this in the tendency to overmedicate people in the mental health system.
The separation from mainstream healthcare also allows for a certain amount of medical shunning. People with mental health and addiction problems can be self-destructive, edgy, difficult, noncompliant, willful or just plain strange. Separated systems make it easy for medical doctors to minimize their own accountability, and kick responsibility over to someone else.
The mainstream medical system is not some add-on or accessory to psychiatric care or addiction treatment. It’s the other way around.
That work helped me to focus more on the question of integrated care. Poor social choices and bad public policy have caused mental health and addiction care to develop like separated orphan twins.
Mental health and addiction are both biopsychosocial, with biological, psychological, and social aspects that continuously reinforce each other and cannot be easily separated, but the treatment systems are separated. Over the course of decades, each system figured out how to emphasize and advocate for its particular service delivery style, treatment philosophy, and culture of care.
This has caused clinicians to develop blind spots. People come away with a different diagnosis and different treatment depending on the system they walk into.
The separation has affected the overall health of the population using mental health and addiction services. We see this in the resistance of addiction treatment systems to medicine-assisted addiction treatment. We also see this in the tendency to overmedicate people in the mental health system.
The separation from mainstream healthcare also allows for a certain amount of medical shunning. People with mental health and addiction problems can be self-destructive, edgy, difficult, noncompliant, willful or just plain strange. Separated systems make it easy for medical doctors to minimize their own accountability, and kick responsibility over to someone else.
The mainstream medical system is not some add-on or accessory to psychiatric care or addiction treatment. It’s the other way around.
Oct 1, 2014
The Smell of Heroin and Snake Oil
 There's a quaint old-fashioned smell of snake-oil around addiction treatment in Kentucky. Kentucky is the center of the heroin epidemic, but its top investment in addiction care isn't, formally speaking, addiction treatment. It is a housing program with peer support, group meetings, and workbooks.
There's a quaint old-fashioned smell of snake-oil around addiction treatment in Kentucky. Kentucky is the center of the heroin epidemic, but its top investment in addiction care isn't, formally speaking, addiction treatment. It is a housing program with peer support, group meetings, and workbooks. Recovery Kentucky, the program that builds recovery centers across the state, uses a non-medical model from the Healing Place in Louisville, a model that is used in other states to side-step the formalities of science-based addiction care. The program is not physician-supervised, and does not follow a medical model. People with chronic pain or medication needs cannot be served in the program.
For heroin, the National Institute of Drug Abuse recommends Medication Assisted Treatment and cognitive behavioral therapy. Recovery Kentucky uses neither. It relies on peer group meetings, and "trudging."
“Trudging is an important part of the Recovery Kentucky Program. When an addict is in the midst of their addiction, they will go to any extreme to get their drug of choice. Once they have entered into the program, they are asked to have that same dedication to achieving their recovery. All recovery centers have their MT classes in off-site locations that the clients walk to and from. Clients generally walk two-to-four round-trip miles a day, based on location. The only time participants do not trudge is if the weather or conditions pose a danger to them—not an inconvenience but a danger, such as an ice storm or tornado. Recovery Kentucky participants can be seen walking in the heat of summer, the leaves of fall, the snow of winter, or the rain of spring. “Now don't get me wrong. There are people who respond well to this sort of program. I have met many people who have rebuilt their lives after their experience in Recovery Kentucky.
But only about one in three or four individuals who enter these facilities make it through the program The rest wash out in the first few weeks of the program. They do not make it to the point of entry to "Phase One" (which is actually the fourth step of Recovery Kentucky's five-phase program). All of Recovery Kentucky's success statistics are based on people who have made it to this fourth step in their process.
Kentucky needs programs that help the other 70 to 75 percent of people who are stuck on heroin, the ones who cannot trudge through the Recovery Kentucky process. And fast. When people fail programs like these, they always relapse --- and relapse is when heroin is most fatal.
Sources
Designed not to be treatment
http://www.treatmentmagazine.com/newswires/481-the-healing-place-looking-to-expand-model-to-west-virginia-.html
The Healing Place Huntington is far from the first center to try a "regulatory arbitrage" approach to get around expensive licensure requirements by employing a non-medical model, thus asserting in fact not to be a treatment center as defined by state regulatory codes.Trudging
http://www.ncsha.org/system/files/Kentucky_Combating_Homelessness.pdf
Recovery Kentucky Guidelines
http://kyhousing.org/Specialized-Housing/Documents/RecKYGuidebook.pdf
Sep 17, 2014
I Am a Fugitive from an Ohio Drug Court
 It is time to reform some of our "reforms." As I visit elements of our mental health and addiction service systems, I am finding out that certain reform efforts are having trouble delivering on their promises. For the people hit by these failures, people with mental health and addiction and their families, this is a scandal that causes as much suffering and death as old-style chain gangs.
It is time to reform some of our "reforms." As I visit elements of our mental health and addiction service systems, I am finding out that certain reform efforts are having trouble delivering on their promises. For the people hit by these failures, people with mental health and addiction and their families, this is a scandal that causes as much suffering and death as old-style chain gangs.
I. DRUG COURT DEBACLE
I spent a day in drug court recently.
What a disappointment. It was an exercise in piling probation violations on top of felony convictions for being an addict.
The court does not offer medication assisted treatment, so it is to be expected that nearly everyone relapses -- which then becomes a new conviction.
I was there with a man who had a 5th degree felony possession conviction for less than a gram of heroin (something actually against the prosecutor’s indictment policy) from two years ago. He’s still on and off the docket, and getting intermittently incarcerated.
What a waste of time and resources – and a profound extended life disruption for this man, who has extensive trauma, anxiety and mood problems, and needs stability, not this.
Everyone else on the docket seemed to be living out the same story.
I hope this was not a typical day for Drug Court. If so it is a system failure. Everyone doing the work seemed appropriately committed to delivering a good result. They just had a tool that was broken, one that doesn't fit heroin.
II. MENTAL HEALTH COURT MADNESS
I met a woman in a peer recovery center last month who is in trouble with her
Mental Health Court because she isn't taking her medication. She has a therapist she visits regularly, and a doctor who is happy with her not using medication, but the court keeps threatening to sanction her unless she starts taking medication.
Even though she is pregnant.
III. THE LIE THAT KILLS
Methadone is the most widely used medication to manage
cravings for heroin and other opiate drugs. It has been used for close to 50
years to stabilize people, especially those who have the most trouble moving
past heroin use. The “market rate” cost of methadone treatment is about $15 per
day. Most people who need methadone can’t afford it unless Medicaid covers this
expense.
In Northern Kentucky, the local methadone clinic wants to
bill Medicaid for its methadone dispensing service, but it can’t. The state has
not set up a way for the clinic to enroll as a Medicaid provider. There is no
code to use for billing, and no fee structure.
The State Medicaid Plan mandates methadone service, but state
officials won’t act. This violates the federal benefit rights of vulnerable
people and puts people’s lives at risk. When the people who have the most
difficulty making progress without medical help are left without options, they
relapse and die.
This part of the Medicaid plan is just a lie that kills.
Sep 8, 2014
The first coherent strategy for the heroin epidemic

My focus this past year has been the heroin epidemic. The result is a book that delivers three things.
- A coherent strategy to manage heroin overdose risk for the population.
- A strong narrative of recovery that supports harm reduction.
- A public policy framework that aligns service systems and creates the necessary infrastructure.
Heroin is an epidemic, a health threat. What has kept us from attacking it effectively is a social stance we have taken towards the people who suffer. We face a decision point. We can attack it with all we've got. Our health system and legal system can align their efforts, work together, and solve this. Or we watch more people die.This is a book for personal recovery, for advocacy, and for system building work. From the chapter "Social Infection"
Alignment and continuity matter. The fatal risk around heroin is frighteningly high, and people who use heroin are fragile. When people disconnect from service systems, relapse turns fatal fast.
Heroin is proving to be a kind of signaling system. It shows us how shunning, exclusion, violence, neglect, and system failure infect our safe world. This population is tough to serve, but so what. People in service systems have the capacity to adapt, and a duty to respond to the people at the heart of their missions.Purchase SHARP Stop Heroin and Rescue People at Amazon
I have also started a meetup group to pursue development of systematic rescue in communities. Learn more at http://www.sharpstopheroin.com The website also features downloadable worksheets for community planning work.
The book addresses several audiences: community workers, people pursuing recovery and family members, and all the rest of us. The real alternative to heroin is a positive, safe world. It is our efforts, how we treat each other as well as the opportunities we create, that build and sustain that world.
Jul 22, 2014
Kentucky Medicaid Plans Restrict Addiction Care
 In Kentucky, efforts to combat widespread opiate addiction and heroin poisoning deaths are hitting limits built into Kentucky's newly-expanded Medicaid system. A big part of the answer to this epidemic is access to medication that helps stabilize patients while they receive treatment or wait for further care. Unfortunately, Kentucky's new Medicaid system is built on a health insurance infrastructure that can be fairly unfriendly to families with chronic care needs.
In Kentucky, efforts to combat widespread opiate addiction and heroin poisoning deaths are hitting limits built into Kentucky's newly-expanded Medicaid system. A big part of the answer to this epidemic is access to medication that helps stabilize patients while they receive treatment or wait for further care. Unfortunately, Kentucky's new Medicaid system is built on a health insurance infrastructure that can be fairly unfriendly to families with chronic care needs.American healthcare has evolved into a gatekeeper-driven system. Insurers save money by rationing care and by putting barriers in the way of care. All of this is calculated. Companies know that when service becomes inconvenient, a certain number of people will simply give up, and the company will never have to pay. The extent to which a company puts self-interest ahead of patient interest is embodied in its published plan documents, regulatory filings, and customer service practices.
The preferred drug list or formulary is a list of medications a plan intends to pay for. The plan might eventually approve or pay for others on a case-by-case basis, but customers who need medicines that are not on these lists should expect to encounter obstacles. This is intentional. Companies know that drug formularies are interpreted as a reflection of company attitudes towards patients with various specific healthcare needs. Insurers manipulate formulary listings to discourage certain patients from enrolling in their plans. In public benefit situations like Medicaid or Medicare, insurers are paid for managing a certain population’s health risk – and the higher the risk of the patients they enroll, the lower the company's bottom line.
Here’s how these factors impact patient care for addiction in Kentucky. The three medications which are FDA approved for Medication Assisted Treatment for opiate and heroin addiction are Methadone, Suboxone, and Vivitrol.
Kentucky has five Medicaid Managed Care Organizations. I tracked down each company's online drug formularies/preferred drug lists, and discovered the following.
- One provider lists only Methadone.What I read from this is that only one of the companies seems willing to support all the available medication options. You can draw your own conclusions.
- Another lists only Suboxone.
- Two providers list two of the three medications: Methadone and Suboxone.
- Only one lists all three: Methadone, Suboxone, and Vivitrol.
If you or your family's health depends on Kentucky Medicaid
You can start your own research journey at this link.
Companies update formularies periodically, so perhaps the situation will change. Kentucky requires managed care organizations to post their plan documents online, but as of today it does not offer plan-by-plan comparison tools. Medicaid representatives say customers who are denied services under any of the plans have appeal rights, but to me that's just another built-in obstacle. Folks at high risk need prompt care.
People who find out that they are stuck on the wrong managed care plan can switch from one plan to another, even after the open enrollment period ends, using a process described here.
More information about Kentucky Medicaid managed care enrollment is found here.
---
Meet me August 6th to talk about what it will take to stop heroin deaths, at the Cincinnati SHARP Stop Heroin Meetup. Learn more.
Jul 12, 2014
My System Reform Wishlist
What might really improve behavioral health? The Ohio Mental Health and Addiction Service Department has a survey out, looking for input.
Here are the key survey questions, and what I wrote.
1. Briefly describe the top 5 issues (in rank order) that, if addressed, would have a significant impact on the lives of persons with substance abuse challenges in your community?
1 Establish a clear path to safety and good health, and align system resources to support that path
2 Eliminate system-created barriers, delays and disincentives
3 Foster population-level nonclinical social support and volunteer-delivered service networks
4 De-emphasize pathology thinking (e.g. AA), emphasize personal strengths, learning, improved cognition, improved relationships, and safe environments
5 Align justice system practices with the path to safety and good health
2. Briefly describe the top 5 issues (in rank order) that, if addressed, would have a significant impact on the lives of persons with mental health challenges in your community?
1 Establish a clear path to safety and good health, and align system resources to support that path
2 Eliminate system-created barriers, delays, and disincentives
3 Establish population-level nonclinical social support and volunteer-delivered service networks
4 De-emphasize pathology thinking (e.g. personal identity connected to clinical diagnosis), emphasize personal strengths, learning, improved cognition, improved relationships, and safe environments
5 Align justice system practices with the path to safety and good health
3. Do you have specific ideas about how to address the issues you mentioned in questions 1 & 2? Please explain:
For a variety of reasons, our systems pay lip service to the notion that behavioral health is biopsychosocial. We only invest in biological methods. We underfund the psychological, and ignore social support completely. This imbalance creates failure, because we are trying to solve population level problems with the most expensive techniques imaginable. Our system has developed a siege mentality. It is plain from reading community plans that system leaders mostly look inward, fretting over the little resources they have. The system must start facing outward, and figure out ways to serve the whole population effectively. This means that, instead of acting like 88 service fortresses in 88 service deserts, the system needs to act more like a network of service hubs. If the system can’t support funding a particular technique (e.g. medication assisted treatment for addiction), it should remove the service from the behavioral health carve-out, and find ways to collaborate with systems that can support the technique. There should always be a path to the least expensive, most accessible way to deliver what is needed when it is needed. People should feel safe and connected if they must wait for a more intensive service.
The relevant techniques for redesigning effective service systems are community organizing, appreciative inquiry, civic engagement, asset based community development, and the IDEO Human Design toolkit.
I developed NAMI Ohio’s court and jail training, worked on the Hamilton County SAMI team. I have developed crisis de-escalation training, and worked on tough issues in multiple service systems. I have been working and learning from Peter Block and other civic engagement experts about how to generate positive solutions to seemingly intractable problems. I do licensing and accreditation work for service delivery agencies. For the past several years I have focused on what ordinary people can do to support each other, and writing about how to change the experience of having mental illness. I have written a well-regarded book that embodies what I have learned. For the past year, I have also worked with anti-drug advocacy groups in Northern Kentucky about heroin poisoning issues. I have learned that it is possible to articulate a path to safety and good health that is practical, understandable, consensus based, and effective.
4. Who would you need to partner with in your community in order to effectively address the issues you mentioned in questions 1 & 2?
Behavioral health is a population-level issue. The whole community has a stake in it. Effective system reform will come from engaging business leaders, neighborhood groups, church groups, parent groups, service system users and political leaders. Today’s reforms are mostly about responsiveness and clarity, not about delivering a smidgen more of what the current system cannot deliver.
5. Briefly describe what the impact would be to your community if these issues were addressed?
People with substance abuse issues – particularly heroin – would move from having a life that is unsafe, at risk of harming others, and is essentially criminal, to a life of a person who is enrolled in a system, who has first aid available, who is safe from infection, whose life is managed, not criminal, less risky, positive, supported and safe. People with mental illness would retain economic and social capacity, move from social isolation and control by others to a life that is safe, socially supported, with access to care as needed, delivered in an ethical, collaborative fashion, and oriented to achieving the ordinary milestones of human development.
---
Photo By Carin fuerst (Own work) [CC-BY-SA-3.0-at (http://creativecommons.org/licenses/by-sa/3.0/at/deed.en)], via Wikimedia Commons
Here are the key survey questions, and what I wrote.
1. Briefly describe the top 5 issues (in rank order) that, if addressed, would have a significant impact on the lives of persons with substance abuse challenges in your community?
1 Establish a clear path to safety and good health, and align system resources to support that path
2 Eliminate system-created barriers, delays and disincentives
3 Foster population-level nonclinical social support and volunteer-delivered service networks
4 De-emphasize pathology thinking (e.g. AA), emphasize personal strengths, learning, improved cognition, improved relationships, and safe environments
5 Align justice system practices with the path to safety and good health
2. Briefly describe the top 5 issues (in rank order) that, if addressed, would have a significant impact on the lives of persons with mental health challenges in your community?
1 Establish a clear path to safety and good health, and align system resources to support that path
2 Eliminate system-created barriers, delays, and disincentives
3 Establish population-level nonclinical social support and volunteer-delivered service networks
4 De-emphasize pathology thinking (e.g. personal identity connected to clinical diagnosis), emphasize personal strengths, learning, improved cognition, improved relationships, and safe environments
5 Align justice system practices with the path to safety and good health
3. Do you have specific ideas about how to address the issues you mentioned in questions 1 & 2? Please explain:
For a variety of reasons, our systems pay lip service to the notion that behavioral health is biopsychosocial. We only invest in biological methods. We underfund the psychological, and ignore social support completely. This imbalance creates failure, because we are trying to solve population level problems with the most expensive techniques imaginable. Our system has developed a siege mentality. It is plain from reading community plans that system leaders mostly look inward, fretting over the little resources they have. The system must start facing outward, and figure out ways to serve the whole population effectively. This means that, instead of acting like 88 service fortresses in 88 service deserts, the system needs to act more like a network of service hubs. If the system can’t support funding a particular technique (e.g. medication assisted treatment for addiction), it should remove the service from the behavioral health carve-out, and find ways to collaborate with systems that can support the technique. There should always be a path to the least expensive, most accessible way to deliver what is needed when it is needed. People should feel safe and connected if they must wait for a more intensive service.
The relevant techniques for redesigning effective service systems are community organizing, appreciative inquiry, civic engagement, asset based community development, and the IDEO Human Design toolkit.
I developed NAMI Ohio’s court and jail training, worked on the Hamilton County SAMI team. I have developed crisis de-escalation training, and worked on tough issues in multiple service systems. I have been working and learning from Peter Block and other civic engagement experts about how to generate positive solutions to seemingly intractable problems. I do licensing and accreditation work for service delivery agencies. For the past several years I have focused on what ordinary people can do to support each other, and writing about how to change the experience of having mental illness. I have written a well-regarded book that embodies what I have learned. For the past year, I have also worked with anti-drug advocacy groups in Northern Kentucky about heroin poisoning issues. I have learned that it is possible to articulate a path to safety and good health that is practical, understandable, consensus based, and effective.
4. Who would you need to partner with in your community in order to effectively address the issues you mentioned in questions 1 & 2?
Behavioral health is a population-level issue. The whole community has a stake in it. Effective system reform will come from engaging business leaders, neighborhood groups, church groups, parent groups, service system users and political leaders. Today’s reforms are mostly about responsiveness and clarity, not about delivering a smidgen more of what the current system cannot deliver.
5. Briefly describe what the impact would be to your community if these issues were addressed?
People with substance abuse issues – particularly heroin – would move from having a life that is unsafe, at risk of harming others, and is essentially criminal, to a life of a person who is enrolled in a system, who has first aid available, who is safe from infection, whose life is managed, not criminal, less risky, positive, supported and safe. People with mental illness would retain economic and social capacity, move from social isolation and control by others to a life that is safe, socially supported, with access to care as needed, delivered in an ethical, collaborative fashion, and oriented to achieving the ordinary milestones of human development.
---
Photo By Carin fuerst (Own work) [CC-BY-SA-3.0-at (http://creativecommons.org/licenses/by-sa/3.0/at/deed.en)], via Wikimedia Commons
May 25, 2014
Social services, and pots of money
I learned about pots of money in grant proposal writing class.
The instructor showed us four flowerpots, four empty cups, and a watering can. Each cup had a label. Each flowerpot had a label. She poured water from the watering can into each of the cups. Then she matched each cup to each flowerpot, then she poured from each cup into its matching flowerpot.
The instructor said funding social services meant thinking in terms of pots of money. These turned into pots of client service. Enough pots, and the agency could sustain its work.
This lesson was absolutely true. My boss at Catholic Social Services often talked in terms of pots of money. A pot of money meant a pot of agency resources to put staff people in jobs. Each pot let our agency address a certain kind of trouble. One problem, one service, one flowerpot. Our agency was a tray of flowerpots, funded with matching pots of money.
People in service agencies have adapted to pot-of-money thinking. We analyze each person looking for service who walks through our doors, identify each person’s list of problems, match the problems to pots of money, and deliver whatever services might match. And only those services. What we deliver is always hit-or-miss.
The truth is that our pot-of-money system is perfectly designed to deliver hit-or-miss services. It does that every day, even though the process started with all the resources in a single watering can.
Is there a way to ditch the cups and flowerpots, give up on matchy-matchy pot-of-money thinking, and start a real garden instead?
---
Photo Rod Allday [CC-BY-SA-2.0 (http://creativecommons.org/licenses/by-sa/2.0)], via Wikimedia Commons
The instructor showed us four flowerpots, four empty cups, and a watering can. Each cup had a label. Each flowerpot had a label. She poured water from the watering can into each of the cups. Then she matched each cup to each flowerpot, then she poured from each cup into its matching flowerpot.
The instructor said funding social services meant thinking in terms of pots of money. These turned into pots of client service. Enough pots, and the agency could sustain its work.
This lesson was absolutely true. My boss at Catholic Social Services often talked in terms of pots of money. A pot of money meant a pot of agency resources to put staff people in jobs. Each pot let our agency address a certain kind of trouble. One problem, one service, one flowerpot. Our agency was a tray of flowerpots, funded with matching pots of money.
People in service agencies have adapted to pot-of-money thinking. We analyze each person looking for service who walks through our doors, identify each person’s list of problems, match the problems to pots of money, and deliver whatever services might match. And only those services. What we deliver is always hit-or-miss.
The truth is that our pot-of-money system is perfectly designed to deliver hit-or-miss services. It does that every day, even though the process started with all the resources in a single watering can.
Is there a way to ditch the cups and flowerpots, give up on matchy-matchy pot-of-money thinking, and start a real garden instead?
---
Photo Rod Allday [CC-BY-SA-2.0 (http://creativecommons.org/licenses/by-sa/2.0)], via Wikimedia Commons
May 1, 2014
The Service Fortress in the Service Desert
I have been reading through a collection of community mental health plans, shocked and disappointed by the number of people that Ohio’s state and county governments have written off.
Our mental health service system has become a fortress in a desert. Sentries guard the doors. Leaders signal for help and unload supply wagons, but hesitate to let people inside.
This makes no sense in modern times. There is no special magic in a walled-up system. People who need mental health services are dispersed throughout our society. They need help where they are.
Ohio has a system of county mental health boards, whose mission is to look out for what the population needs. Read enough community health plans, and you’ll see the siege mentality that has taken hold. Planners count survivors and fret about what's left inside the fortress walls.
In Hamilton County, where I live, the poverty rate has climbed from 10.8 percent to 18.5 percent from 2002 to 2011. This factor alone drives increased rates of depression and dysfunction, but our county public system does not address this. The county planners write.
The implications of “no service” are predictable. People suffer. Families suffer. There’s economic damage, career disruption, more poverty, more drug abuse, more crime, more violence, more failure.
What our planners write about the downside of “no service” is this.
There’s a lot of noise and self-congratulation this Mental Health Month. Pay no attention. The people in the service fortress are whistling in the wind. The service system needs a good wallop of retargeting and reform Read the service plan before you buy the ticket to the gala.
---
Ohio’s community mental health service plans can be found at this link.
http://mha.ohio.gov/Default.aspx?tabid=153
---
photo © Dr Michel Royon / Wikimedia Commons
Our mental health service system has become a fortress in a desert. Sentries guard the doors. Leaders signal for help and unload supply wagons, but hesitate to let people inside.
This makes no sense in modern times. There is no special magic in a walled-up system. People who need mental health services are dispersed throughout our society. They need help where they are.
Ohio has a system of county mental health boards, whose mission is to look out for what the population needs. Read enough community health plans, and you’ll see the siege mentality that has taken hold. Planners count survivors and fret about what's left inside the fortress walls.
In Hamilton County, where I live, the poverty rate has climbed from 10.8 percent to 18.5 percent from 2002 to 2011. This factor alone drives increased rates of depression and dysfunction, but our county public system does not address this. The county planners write.
Due to limited resources, there is limited capacity for outpatient counseling for those clients who do not have a severe and persistent mental illness.In practice, “limited capacity” means “no service.”
The implications of “no service” are predictable. People suffer. Families suffer. There’s economic damage, career disruption, more poverty, more drug abuse, more crime, more violence, more failure.
What our planners write about the downside of “no service” is this.
The limited capacity for outpatient counseling for clients who do not have a severe and persistent mental illness could result in the use of more costly Medicaid and non-Medicaid services.And
Untimely access to pharmacological services for children and families due to the shortages in child psychiatry services may result in more rapid decompensation in children’s functioning which could lead to more utilization of inpatient services, out of home placements, and other costly interventions.And
Gaps in access for low income populations, lack of resources for housing, medication and long term residential services, ultimately impacts the AOD [Alcohol Or Drug] client either using jail bed days, hospital days or death. This is a high cost for the community.Ohio’s mental health system is self-focused, inward looking, not community focused. It chooses not to adapt. It chooses to live under siege, when it might focus on collaboration, and on creating seamless networks of service that permeate communities.
There’s a lot of noise and self-congratulation this Mental Health Month. Pay no attention. The people in the service fortress are whistling in the wind. The service system needs a good wallop of retargeting and reform Read the service plan before you buy the ticket to the gala.
---
Ohio’s community mental health service plans can be found at this link.
http://mha.ohio.gov/Default.aspx?tabid=153
---
photo © Dr Michel Royon / Wikimedia Commons
Apr 30, 2014
SHARP Stop Heroin And Rescue People
Heroin is today's plague of dead children. As David Pepper points out in this post on his website, Town Hall meetings will not solve the heroin crisis. We must act urgently to defeat this epidemic. The solution involves reducing demand through prevention and treatment, while law enforcement targets trafficking and violence.
By the way, David has been working on connecting health care with justice for a long time. Many of the practices starting to be implemented in jails across the US connect with David's initiatives in Hamilton County when he served as County Commissioner. Our county was one of the first to suspend, not terminate, Medicaid benefits for prisoners in jail. This helped us connect released prisoners to treatment for mental health and addiction care. This was a bipartisan effort. Everyone benefits from a safer, healthier community.
David has the plan. Let me offer an acronym. SHARP Stop Heroin And Rescue People.
---
My prior posts on the heroin crisis
Apr 28, 2014
Local paper prints old news about me
I am one of the first people in the mental health recovery community to run for a substantial public office, so it's not surprising that the local paper would find this interesting. Today, the Cincinnati Enquirer published a story about me, headlining my law license suspension 16 years ago.
The real story about my life is not about my falling down. It is about my recovery, and the work I have done since then to improve people's lives. The man who prosecuted my law license discipline case agrees. Last year, when the Enquirer published a suicide prevention article I wrote, this gentleman sent me a note.
Here is the message I sent back to Bob Laufman.
If anyone wants to have a chat about all this, call my campaign phone number. (513) 494-6280.
The real story about my life is not about my falling down. It is about my recovery, and the work I have done since then to improve people's lives. The man who prosecuted my law license discipline case agrees. Last year, when the Enquirer published a suicide prevention article I wrote, this gentleman sent me a note.
I have often thought of you and wondered what had happened to you after your suspension. I observed your transformation from the time of your deposition throughout your diagnosis and argument in the Ohio Supreme Court. I was amazed at how well you argued. You established that while mental illness is not a complete defense it can be use in mitigation. It is still the landmark case on the subject.
I am sorry you could not return to law but you can do more good and help more people in need that you ever could as an attorney. I hope you and your family are happier now as a result of your change. I am proud that you dug yourself out of what I feared was an insurmountable hole. I am delighted that you are doing so well. Congratulations.
Kathy was a psychiatric social worker and for many years has been co-chair of GLSEN working with schools to prevent bullying which often lead to suicides She also has a younger sister who is bipolar so we have a special interest in the work your are doing.
I am now retired and living in a condo. We would welcome hearing from you but understand if you never want to hear from me again.My story has not been hiding. It is part of my Amazon profile, and my Blogger profile. The court decision is on the Ohio Supreme Court website. The local Bar Association and the Ohio Supreme Court have funded my work. The recovery process I describe in my book and on this blog is what helped me. The local Bar Association knows I have spoken with other lawyers who have been dealing with mental health issues. And these days, I do campaign finance work for judges.
Best wishes.
Bob Laufman
Here is the message I sent back to Bob Laufman.
Bob
Thank you so much for your kind note. I just read it aloud for my wife. It made my day. I always understood you had a role to play. I've been at peace with it all for many years.
For years I have considered myself the poster child for the do-gooder kicked out lawyer. I attribute my recovery to the unwavering support of my family, the right diagnosis and treatment, and the willingness of people to send me opportunities. I've considered ways to normalize my status, perhaps transitioning from ‘suspended’ to ‘retired’ or some sort of restricted practice where I could do some public policy work or teach, but I never thought it worth the effort. I should probably go after it, just to complete the story.
I have always done justice-connected work, starting in the late 1990s when I designed the website for the Collaborative Law group and the Center for Mediation of Disputes. I was on the SAMI initiative, one of the early mental health jail diversion initiatives, from 1998-2003. In 2000--2001 I wrote the NAMI Ohio mental health training curriculum for courts and jails. I took that training across the state and to Kentucky, where it became mandatory for deputy jailers across the state, part of a jail suicide prevention initiative. I wrote a NAMI policy paper on the Olmstead decision, and authored a guardianship support program. I've been Nadine Allen's campaign treasurer for the past two campaigns. Now I am doing that with Ted Berry Jr.
Would you be interested in doing some sort of programming around mental health and recovery in the profession? I have no idea where the law has gone since my case came up, but I’m interested in having a real dialogue about it. It’s time for me to tell my story.
Finally, what I remember most about the Supreme Court hearing was the number of people who talked about being inspired by the character Atticus Finch. I have always considered him a false hero. My hero is Boo Radley, the outsider guy who really saved the lawyers kids.
Please call me any time. My home number is ....
If anyone wants to have a chat about all this, call my campaign phone number. (513) 494-6280.
Apr 27, 2014
Mobilizing medical warriors to stop heroin

Heroin Plan In A Nutshell
In the Greater Cincinnati region, we have most of the infrastructure needed to create a pipeline that enrolls addicts while they are still using drugs, makes their lives safer, and conducts them along a path to safety and rescue from addiction. The next step is to enroll doctors and healthcare institutions, and form a coalition of the willing to wage war on the heroin epidemic that steals lives daily throughout our region.
In the past week, I have spoken with health educators at Cincinnati Children’s Hospital and the Cincinnati Health Department, an administrator at the local Recovery Services Board, the head of a local treatment provider agency, community members concerned about a proposed needle exchange program, anti-drug educators, and dozens of street outreach workers and health communicators participating in our region’s largest and most significant annual urban health outreach event.
I learned that:
We need to recruit dozens of physicians who are each willing to care for 30 addiction medication patients annually.
We need to recruit hospital systems to house and support these physicians.
We need to connect the public drug treatment system (which is funded to supply medication for addiction treatment) with physicians who are funded to provide medical supervision in neighborhood primary care clinics (FQHCs) and other healthcare settings.
We need to connect paramedics and health educators with sources of the first aid drug for overdoses, so this resource becomes available throughout the community the same way automatic defibrillators are available to stop heart attacks.
We need high level leadership – those who are willing to talk outside of their “funding gutters” and connect up their systems – to meet each other and declare their commitment to stop this epidemic by every means within their power.
Read my earlier post:
Apr 25, 2014
Chatter from young psychiatrists
I stumbled on a message board for young doctors, offering a treasure trove of anecdotes about the current state of psychiatric practice. The issue at the start of the March 2014 conversation was a doctor who felt threatened by an influx of nurse practitioners (NPs). Medical doctors have significantly more training than NPs, but the economics of psychiatric practice may not reflect that differential. The conversation veers off into a discussion of the standard of care that patients demand, or are entitled to.
This is a mere bundle of anecdotes, to be sure, but a fascinating bundle. I've clipped bits and pieces from the discussion thread. It's pretty raw for doctor talk.
---
Source:
http://forums.studentdoctor.net/threads/current-practice-environment.1057875
This is a mere bundle of anecdotes, to be sure, but a fascinating bundle. I've clipped bits and pieces from the discussion thread. It's pretty raw for doctor talk.
---
With what I see the psychs are seeing more patients an hour. My guess is that there are a couple reasons for this:---
1) the pt is likely to get even more upset if a nurse rushes them in an out in med check style in less than 5 minutes. If someone who is an md does it, they may just assume that is what md's get to do or whatever. But if a nurse treats them that way....(again not saying it's right, but that may be the perception)
2) the psych(competent ones at least) is more likely able to practice whack and stack psychiatry because they usually can identify obvious pharmaco no-no's quicker almost as a reflex, whereas the psych np may have to think about those things for a second. So in a way the greater fund of knowledge of the psych allows them to practice relative safe whack and stack psychiatry easier.
I can't solve all the mental health problems.---
But I can help the people who want my help and appreciate it.
I think people in medicine come from pretty sheltered (and generally affluent) backgrounds, which can limit our work with our patients.---
The nurse practitioner question---
Replying to "As far as the public goes, they can suck it. They benefit from residents keeping the lights on in Americas hospitals then then they can pay for it. It and the years of effort and sacrafice it takes to make a doc. They want to replace us. F@ck them"
Unfortunately, doctors being entitled and telling the public they treat to just suck it is one of the reasons we're fighting the things we're fighting.
This post makes me think about crossing psychiatry off the list of potential specialties. Only 1% from my school choose psychiatry in the last match, and I can't see how anecdotes of NP's replacing psychiatrists will do anything except scare off more med students and make psych even more unpopular.---
The argument that psychiatrists don't have to worry about their jobs because they add more value than an NP would be laughable to a hospital MBA, owner of a practice group, or insurance exec. Adding value means adding money to the bottom line. NP's add more value than a psych if they cost less but generate the same amount of revenue and have the same malpractice risk.
Seems like the only people who care about "quality" are the very small subset of patients who can do cash pay. Otherwise, the general public has no say on the quality and value of their psych because their 3rd party payer dictates what is "value". The public only cares that someone in a white coat accepts their insurance, can see them in a timely manner, and won't kill them. It's a low standard that NP's can fulfill, just like the masses of IMG's and assorted folks who couldn't match into anything else are doing now.
I haven't followed this whole thread so I apologize if I'm repeating anything. But I just wanted to jump in, because the issue about NPs interests me. I started a job last summer after finishing residency. It's mostly outpatient with some inpatient coverage. Overall it's going pretty well. Certainly it's an improvement upon the horrors of residency. But my fellow psychiatrists here each supervise one if not more NPs, and their NPs cover the inpatient unit too. Sometimes I come on call after them, and am then asked to discharge patients the NPs have admitted and followed. The thing is, they make some astonishingly poor medication choices and their notes are the worst notes I've ever seen. At times it's impossible even to understand why they are in the hospital and what has been done. So when I have to discharge these patients I am pretty nervous. They no longer meet commitment criteria and I end up having no choice. I try to document that I recommend they stay in the hospital and recommend they try medication X or whatever instead of whatever they're on, but I imagine this documentation only will protect me so far. Last week I had a patient bounce back after such a discharge. The guy was taking 20mg q4h PRN of zyprexa for anxiety. Yes, that was one of his meds. And risperdal BID. There was no good reason mentioned as to why. Obviously I did not continue the PRN zyprexa when he left. But I don't know if the antipsychotic effect was actually helping? There sure were no notes to guide me. The diagnosis wasn't consistent or justified by his presentation.---
I do think the NPs have a good rapport with patients and I'm not trying to discredit them, but I worry about my own liability coming on after them. There's no way I'll bring this up with my colleagues - I'd quit before I'd confront them because I suspect they'll be defensive, not to mention they'll have illogical justifications rationalizing how they are "working with" the NPs, and I don't want to hear it. Plus I'm in a different part of the country than where I did residency, and the medication philosophies seem to be different here. Not that it was perfect where I was for residency, of course. But even from local psychiatrists I'm seeing these gigantic doses of layered on antipsychotics, and a lot of polypharmacy. Benzos and adderall are big. Psychotherapy is done by social workers largely and from what I hear, most patients aren't big fans. Can you blame them? Maybe it's because I'm not in an academic environment, maybe that's the problem. But academia has its problems too...
1) Psychiatrists don't come up with differential diagnoses. Internists do. In psychiatry we have about 10 or so conditions we routinely use, and almost invariably the patient gets fit into one of those 10 or so, rather than a genuine process of "differential diagnosis" occurring. If you disagree then tell me the last time you made a serious list in your "assessment" section of what the problem could be, and what specific diagnostic tests, procedures, or observations you were going to do to "rule out" some of the possibilities and "rule in" others.
2) Risk assessments in real life are boilerplate. They are written with the intention of justifying whatever decision was made. They are not written and then used to make decisions.
3) Dispo arrangements should have already been done by social work.---
I disagree with the differential comment. I think working through a DDx both in your head and in your notes is a useful exercise, and can help keep your mind open to different (and maybe less likely) possibilities. Probably most useful with a new patient with no known psych history. Also useful on consults, and with patients who may or may not have a personality disorder clouding their picture. I think dismissing the entire approach of using a differential (at least for difficult or complex cases) is throwing away a useful tool and strikes me as pretty sloppy. You could miss some important stuff (i.e. that "easy" case was actually complicated by heavy substance use that nobody knew about, or that simple delirium consult had focal neuro findings from a brain met that nobody really checked for).---
For those of us with more experience, the differential is usually fairly simple - when I admit a psychotic patient (psychosis nos) I know that I will probably need to start an antipsychotic and if the precise dx is not known, start the work up (or suggest the workup if it is a weekend and there aren't SW's around to help)- get collateral history/check labs/get old records. Usually the diff involves primary vs drug-induced, with the rare neurologic/medical etiology. When I admit a pt, I usually spend much more time thinking about their comorbid medical problems (HTN, DM, etc) than the differential. You got to get the patient stabilized and then fine tune the diagnosis during the hospitalization. I am of course talking about psychiatry in an inpatient environment.---
Now not every inpatient falls in the category where it doesn't matter if you work really efficiently and finish it up quickly vs taking a thorough and slow approach, but many do. For every 100 inpatients you see, think about how many are patients where the outcome and/or care isn't going to vary whether you spend x minutes or 4x minutes. A *lot*. At least at the different inpatient places I've worked. Yes, it does take a good bit of time to go over pt education with a low functioning family whose 19yo son is in the hospital for the first time with psychosis. But for every 1 case like that, there are 5-6 that don't have issues where time is required like that.
Now for the most part I don't think inpatient is where patients really get better or where much of anything positive happens....and that's why I'm not going to do it. But if I did do it, I think I would be pretty darn efficient at it.---
Ummm what?? Are you serious about not having a differential diagnoses. I view psychiatric disorders as diagnosis of exclusion. Everyone gets a medical workup and drug screen. Anything less and you are providing substandard care and essentially not using what you should have learned in medical school. Can't say how many times I have pressed this point to medical students and insurance companies that initially deny tests only to approve it after I contact them. I have found tumors on MRIs, (+) syphillis tests, obviously numerous sub induced disorders including bath salts, etc...
People are talking about psych NPs encouragement on psychiatrists and us needing to shorten our training. What needs to happen is that within our own speciality there needs to be a better standard of care. I may poke fun at some NP med management skills, but I am appalled at some of the diagnosis and polypharmacy that is rampant in our speciality and it is quite embarrassing.
Deliver better standard of care and show superior results compared to the NPs.
As far as jobs go, everyone in my program landed a solid job. One has the same setup as ---. 60 min intake, 30 min follow up. 215K.---
Source:
http://forums.studentdoctor.net/threads/current-practice-environment.1057875
Apr 17, 2014
Mainstreaming addiction services: How pharmacy clinics can help put an end to the heroin epidemic
I am tired of hearing tragic stories about heroin deaths. It’s time for action. I’ve spent nearly a year working with Dr. Jeremy Engel and advocacy groups from Northern Kentucky working on this problem. I have done my homework. Here’s my approach.
1. Treat heroin as an epidemic, a health threat, with social side effects.
Throughout history, addiction was treated as a social problem, not a health care issue. Now we must adjust the War on Drugs to make it less of a War on Addicts. We want to save our sons and daughters. We have learned we cannot make much progress if all we do is shun and imprison people. Nowadays, we have medical approaches. Here’s what’s in the arsenal.
Healthcare has an open door in every community, with protocols, privacy regulations, security set-ups, connections to regulators, connections to law enforcement, and connections to the broader economy. What might we accomplish if the healthcare system treated addiction and heroin death prevention like every other health concern? We might start with needle exchange in every place that sells flu shots. Every visit is a way to distribute Naloxone. Every visit can connect people who want to stop using drugs with treatment.
3. Work with the willing.
Not everyone is comfortable working with addicted populations, but many of us are. We must ask more groups to sign on. For example, is Kroger willing to sign on, and put Naloxone and needle exchange in its retail clinics?
4. Attend to risk.
Healthcare groups have risk management procedures in place. We see them whenever we stand in line at a grocery store pharmacy. People with drug problems are with us everywhere in our community. They bring with them real risks, but we can address them. If we do, we can make progress on this epidemic of death.
----
Photo by Unknown photographer [Public domain], via Wikimedia Commons
1. Treat heroin as an epidemic, a health threat, with social side effects.
Throughout history, addiction was treated as a social problem, not a health care issue. Now we must adjust the War on Drugs to make it less of a War on Addicts. We want to save our sons and daughters. We have learned we cannot make much progress if all we do is shun and imprison people. Nowadays, we have medical approaches. Here’s what’s in the arsenal.
- Naloxone. Heroin kills by suppressing respiration. Naloxone neutralizes heroin, and restores breathing. It costs $65 for a rescue kit.
- Methadone, Suboxone, and Vivitrol. These three drugs do not stop addiction, but reduce cravings, and help people progress towards recovery. They have good social side effects. They may not stop addiction, but they do stop burglaries and thefts.
- Needle exchanges remove sources of deadly infection from the streets, and provide a pathway to treatment. The risks around needle exchanges can be managed.
- Community support and education. Many anti-drug and health care groups are already on board.
Healthcare has an open door in every community, with protocols, privacy regulations, security set-ups, connections to regulators, connections to law enforcement, and connections to the broader economy. What might we accomplish if the healthcare system treated addiction and heroin death prevention like every other health concern? We might start with needle exchange in every place that sells flu shots. Every visit is a way to distribute Naloxone. Every visit can connect people who want to stop using drugs with treatment.
3. Work with the willing.
Not everyone is comfortable working with addicted populations, but many of us are. We must ask more groups to sign on. For example, is Kroger willing to sign on, and put Naloxone and needle exchange in its retail clinics?
4. Attend to risk.
Healthcare groups have risk management procedures in place. We see them whenever we stand in line at a grocery store pharmacy. People with drug problems are with us everywhere in our community. They bring with them real risks, but we can address them. If we do, we can make progress on this epidemic of death.
----
Photo by Unknown photographer [Public domain], via Wikimedia Commons
Apr 3, 2014
Mental illness, suicide, and violence
I have been written a surprising number of pieces about mental health, suicide, and violence over the course of the past two years. Here’s a list of thirty of these bog posts, arranged (for the most part) in reverse chronological order. My approach is to look at the suicide first, and then the homicide. Fewer than two percent of suicides also involve a homicide.
Adam Lanza’s suicide ignored by state report
http://www.redesigningmentalillness.net/2013/11/adam-lanzas-suicide-ignored-by-state.html
Christian Stenographer’s Rant offers clues to mass violence
http://www.redesigningmentalillness.net/2013/10/christian-stenographers-rant-offers.html
Aaron Alexis and the demon delusion
http://www.redesigningmentalillness.net/2013/09/aaron-alexis-and-demon-delusion.html
What crisis de-escalation really sounds like
http://www.redesigningmentalillness.net/2013/08/what-crisis-de-escalation-really-sounds.html
Is it Kendra’s law, or better care, that helps people get better?
http://www.redesigningmentalillness.net/2013/08/is-it-kendras-law-or-better-care-that.html
Preventing the next bomb plot
http://www.redesigningmentalillness.net/2013/04/preventing-next-bomb-plot.html
Did violent videogames cause the Newtown massacre?
http://www.redesigningmentalillness.net/2013/03/did-violent-videogames-cause-newtown.html
Mentalizing, mental health and the restoration of community
http://www.redesigningmentalillness.net/2013/03/mentalizing-mental-health-and.html
Notes on the PBS After Newtown coverage
http://www.redesigningmentalillness.net/2013/02/notes-on-pbs-after-newtown-coverage.html
Teach suicide prevention wherever people buy guns
http://www.redesigningmentalillness.net/2013/02/teach-suicide-prevention-where-people.html
How to smoke out a suicidal spree killer before anyone gets hurt
http://www.redesigningmentalillness.net/2013/02/how-to-smoke-out-suicidal-spree-killer.html
The Five Step Way to think about Security, Suicide and Guns
http://www.redesigningmentalillness.net/2013/01/the-five-step-way-to-think-about.html
Best comment by a police officer on the ramifications of armed teachers in schools
http://www.redesigningmentalillness.net/2013/01/best-comment-by-police-officer-on.html
Suicide and gun risk are worth checking out
http://www.redesigningmentalillness.net/2013/01/suicide-and-gun-risk-are-worth-checking.html
World's biggest task force, but nobody says anything new
http://www.redesigningmentalillness.net/2013/01/worlds-biggest-task-force-but-nobody.html
Dear Vice-President Biden, Here’s what it takes to fix mental health
http://www.redesigningmentalillness.net/2012/12/dear-vice-president-biden-heres-what-it.html
Vice-President Biden, a few new items for your mental health plan
http://www.redesigningmentalillness.net/2013/01/vice-president-biden-few-new-items-for.html
What I am doing to respond to Sandy Hook
http://www.redesigningmentalillness.net/2012/12/what-i-am-doing-to-respond-to-sandy-hook.html
Frightened moms at the instant before the trigger
http://www.redesigningmentalillness.net/2012/12/frightened-moms-at-instant-before.html
Political correctness in the mental health community is killing people
http://www.redesigningmentalillness.net/2012/12/political-correctness-in-mental-health.html
Coping with a violent child
http://www.redesigningmentalillness.net/2012/12/coping-with-violent-child.html
Mass murder is the new flavor of American suicide
http://www.redesigningmentalillness.net/2012/12/mass-murder-is-new-flavor-of-american.html
Defending Recovery
http://www.redesigningmentalillness.net/2012/12/defending-recovery.html
Don’t Blame Deinstitutionalization
http://www.redesigningmentalillness.net/2012/09/dontt-blame-deinstitutionalization.html
Your hate group, and all our safety
http://www.redesigningmentalillness.net/2012/08/your-hate-group-and-all-our-safety.html
Campus security failures in two mass killings
http://www.redesigningmentalillness.net/2012/08/campus-security-failures-in-two-mass.html
What it takes to prevent mass killings
http://www.redesigningmentalillness.net/2012/07/what-it-takes-to-prevent-mass-killings.html
What’s a risk management person expected to do?
http://www.redesigningmentalillness.net/2012/05/whats-risk-management-person-expected.html
Mental Illness and Crime Prevention
http://www.redesigningmentalillness.net/2012/05/mental-illness-and-crime-prevention.html
Claiming some violent territory for mental illness
http://www.redesigningmentalillness.net/2012/05/claiming-some-violent-territory-for.html
Adam Lanza’s suicide ignored by state report
http://www.redesigningmentalillness.net/2013/11/adam-lanzas-suicide-ignored-by-state.html
Christian Stenographer’s Rant offers clues to mass violence
http://www.redesigningmentalillness.net/2013/10/christian-stenographers-rant-offers.html
Aaron Alexis and the demon delusion
http://www.redesigningmentalillness.net/2013/09/aaron-alexis-and-demon-delusion.html
What crisis de-escalation really sounds like
http://www.redesigningmentalillness.net/2013/08/what-crisis-de-escalation-really-sounds.html
Is it Kendra’s law, or better care, that helps people get better?
http://www.redesigningmentalillness.net/2013/08/is-it-kendras-law-or-better-care-that.html
Preventing the next bomb plot
http://www.redesigningmentalillness.net/2013/04/preventing-next-bomb-plot.html
Did violent videogames cause the Newtown massacre?
http://www.redesigningmentalillness.net/2013/03/did-violent-videogames-cause-newtown.html
Mentalizing, mental health and the restoration of community
http://www.redesigningmentalillness.net/2013/03/mentalizing-mental-health-and.html
Notes on the PBS After Newtown coverage
http://www.redesigningmentalillness.net/2013/02/notes-on-pbs-after-newtown-coverage.html
Teach suicide prevention wherever people buy guns
http://www.redesigningmentalillness.net/2013/02/teach-suicide-prevention-where-people.html
How to smoke out a suicidal spree killer before anyone gets hurt
http://www.redesigningmentalillness.net/2013/02/how-to-smoke-out-suicidal-spree-killer.html
The Five Step Way to think about Security, Suicide and Guns
http://www.redesigningmentalillness.net/2013/01/the-five-step-way-to-think-about.html
Best comment by a police officer on the ramifications of armed teachers in schools
http://www.redesigningmentalillness.net/2013/01/best-comment-by-police-officer-on.html
Suicide and gun risk are worth checking out
http://www.redesigningmentalillness.net/2013/01/suicide-and-gun-risk-are-worth-checking.html
World's biggest task force, but nobody says anything new
http://www.redesigningmentalillness.net/2013/01/worlds-biggest-task-force-but-nobody.html
Dear Vice-President Biden, Here’s what it takes to fix mental health
http://www.redesigningmentalillness.net/2012/12/dear-vice-president-biden-heres-what-it.html
Vice-President Biden, a few new items for your mental health plan
http://www.redesigningmentalillness.net/2013/01/vice-president-biden-few-new-items-for.html
What I am doing to respond to Sandy Hook
http://www.redesigningmentalillness.net/2012/12/what-i-am-doing-to-respond-to-sandy-hook.html
Frightened moms at the instant before the trigger
http://www.redesigningmentalillness.net/2012/12/frightened-moms-at-instant-before.html
Political correctness in the mental health community is killing people
http://www.redesigningmentalillness.net/2012/12/political-correctness-in-mental-health.html
Coping with a violent child
http://www.redesigningmentalillness.net/2012/12/coping-with-violent-child.html
Mass murder is the new flavor of American suicide
http://www.redesigningmentalillness.net/2012/12/mass-murder-is-new-flavor-of-american.html
Defending Recovery
http://www.redesigningmentalillness.net/2012/12/defending-recovery.html
Don’t Blame Deinstitutionalization
http://www.redesigningmentalillness.net/2012/09/dontt-blame-deinstitutionalization.html
Your hate group, and all our safety
http://www.redesigningmentalillness.net/2012/08/your-hate-group-and-all-our-safety.html
Campus security failures in two mass killings
http://www.redesigningmentalillness.net/2012/08/campus-security-failures-in-two-mass.html
What it takes to prevent mass killings
http://www.redesigningmentalillness.net/2012/07/what-it-takes-to-prevent-mass-killings.html
What’s a risk management person expected to do?
http://www.redesigningmentalillness.net/2012/05/whats-risk-management-person-expected.html
Mental Illness and Crime Prevention
http://www.redesigningmentalillness.net/2012/05/mental-illness-and-crime-prevention.html
Claiming some violent territory for mental illness
http://www.redesigningmentalillness.net/2012/05/claiming-some-violent-territory-for.html
Mar 6, 2014
The Road to Positive
 Just about two years ago I began this blog as a way to explore what ordinary people, nonclinicians, could do to change the experience of mental illness in America.
Just about two years ago I began this blog as a way to explore what ordinary people, nonclinicians, could do to change the experience of mental illness in America.Here is the central lesson.
Everything changes once people give up outmoded, inflexible habits of thinking, start listening to each other, accept responsibility for each other’s health and safety, pay due attention to risk, and start doing what they can to pitch in.
This is one of the hidden lessons within much of today's mental health and public policy literature. I have just finished editorial work on Milt Greek's new book Delusions, Meaning and Transformation. Look for it on Amazon and other online booksellers in the next week or two. Milt has always stood for listening to people who have delusions and hallucinations. His insight is that mixed up thinking and delusions are the brain's way of operating when filtering and perception issues flare up. What's happening is complicated, but the person is experiencing something that is intensely meaningful. This experience is so rich and fascinating or troubling that it often motivates the person to resolve his situation and perhaps even help make the world better. Creating an alliance around this quest or mission may be the best way for family, friends and the treatment team to work through and assist in the tasks of recovery.
Feb 26, 2014
Solving campus mental health
Mental health is all the rage on campus today. I came across this article about mental health activism at the University of Virginia and the cover article from Newsweek about college mental health from mid February.
These articles, and many others, show the disconnect between the population that college systems were designed to serve, and the populations they actually serve today.
When colleges were ivory tower, elitist institutions, in isolated spaces, they operated under a set of cultural assumptions. People would arrive prepared to attend college. There would be a scarcity of college slots. Admission would be competitive. Only the finest minds could have access.
For many years, students did arrive expecting a mental pressure cooker experience. People who could not succeed were systematically removed from the population. There were four exit options: Succeed, flunk out, flake out, drop out.
Today’s college environment differs from the college environment of the past. Instead of serving a select population in an isolated, controlled setting, today’s colleges and universities serve a population that mirrors the population as a whole. There is more economic diversity. There is more diversity with respect to academic preparedness, more diversity of social preparedness, more diversity of health concerns, more diversity of economic preparedness. And more diversity with respect to mental health.
Colleges are learning that the whole population brings all of its trends with it.
What colleges need for mental health is what our whole society needs for mental health: a complete system, one that permeates the population, redesigned to support the whole population.
This means a system that stacks up remedies, starting in families and in informal groups, and then proceeding to organized social, nonclinical experiences, and from there to clinical systems.
We must simplify the conversation. Information overload adds to fear, and mental illness is scary enough. People need enough information to understand what is happening and put together a plan.
Everyone must be encouraged and authorized to do what they can. It's hard to have hope if you're helpless. Every person with symptoms, and every potential ally, needs a way to pitch in. This builds confidence, promotes safety, and makes hope real.
It pays to focus on strengths, not symptoms. Sickness and stigma steal our attention, blinding us to strengths that people retain and to strategies people can use to build capacity.
We must allow recovery to mean something. These days, most people with mental illness regain the capacity to participate in the larger community, and lead a meaningful life. Recovery is social and developmental as well as medical. We deny ourselves a sense of making progress if we over focus on symptom relief. We deny people progress when we do not help them regain their place in society.
We must practice nonstigma. Nonstigma is true inclusion, a belief of the heart that everyone belongs together in the world. Everyone can work on becoming welcoming, tolerant, accommodating. Nonstigma is more than technique. Nonstigma is a virtue.
And so, for colleges, the suicide rate will drop once nearly everyone knows something about suicide prevention. More people will complete college once colleges reform their service delivery and failure systems.
If we want to live in a positive, safe world, we have to embrace the need to create it, and include everyone as we bring the vision forward.
These articles, and many others, show the disconnect between the population that college systems were designed to serve, and the populations they actually serve today.
When colleges were ivory tower, elitist institutions, in isolated spaces, they operated under a set of cultural assumptions. People would arrive prepared to attend college. There would be a scarcity of college slots. Admission would be competitive. Only the finest minds could have access.
For many years, students did arrive expecting a mental pressure cooker experience. People who could not succeed were systematically removed from the population. There were four exit options: Succeed, flunk out, flake out, drop out.
Today’s college environment differs from the college environment of the past. Instead of serving a select population in an isolated, controlled setting, today’s colleges and universities serve a population that mirrors the population as a whole. There is more economic diversity. There is more diversity with respect to academic preparedness, more diversity of social preparedness, more diversity of health concerns, more diversity of economic preparedness. And more diversity with respect to mental health.
Colleges are learning that the whole population brings all of its trends with it.
- Today’s college population includes more women, and therefore colleges are encountering increased rates of depression.
- Today’s college population includes more people who have experienced poverty, and so on campus there are many more people with histories of exposure to so-called “adverse childhood events” – the assortment of tough situations that cause cognitive difficulties and trouble with building social connections.
- Today’s college population includes many recent combat veterans, and therefore more risk of post-traumatic stress disorder.
- Today’s college population still retains its basic age range, young adulthood, the sweet spot for the onset of schizophrenia.
What colleges need for mental health is what our whole society needs for mental health: a complete system, one that permeates the population, redesigned to support the whole population.
This means a system that stacks up remedies, starting in families and in informal groups, and then proceeding to organized social, nonclinical experiences, and from there to clinical systems.
We must simplify the conversation. Information overload adds to fear, and mental illness is scary enough. People need enough information to understand what is happening and put together a plan.
Everyone must be encouraged and authorized to do what they can. It's hard to have hope if you're helpless. Every person with symptoms, and every potential ally, needs a way to pitch in. This builds confidence, promotes safety, and makes hope real.
It pays to focus on strengths, not symptoms. Sickness and stigma steal our attention, blinding us to strengths that people retain and to strategies people can use to build capacity.
We must allow recovery to mean something. These days, most people with mental illness regain the capacity to participate in the larger community, and lead a meaningful life. Recovery is social and developmental as well as medical. We deny ourselves a sense of making progress if we over focus on symptom relief. We deny people progress when we do not help them regain their place in society.
We must practice nonstigma. Nonstigma is true inclusion, a belief of the heart that everyone belongs together in the world. Everyone can work on becoming welcoming, tolerant, accommodating. Nonstigma is more than technique. Nonstigma is a virtue.
And so, for colleges, the suicide rate will drop once nearly everyone knows something about suicide prevention. More people will complete college once colleges reform their service delivery and failure systems.
If we want to live in a positive, safe world, we have to embrace the need to create it, and include everyone as we bring the vision forward.
Subscribe to:
Posts (Atom)